Carbohydrate (Glucose) Tolerance: Definition, Signs, and Lab Test
Carbohydrate (Glucose) Tolerance: Definition, Signs, and Lab Test
As a personalized health optimization company, we believe how much carbs anyone should eat is very individual, so you need to figure out your personal glucose tolerance. After all, optimal blood sugar control is crucial whether you want to:
- Look your best
- Achieve cognitive or physical God mode
- Live a long and healthy life
- Balance your hormones
In this article, we dig deep into the world of carbohydrates to learn what “glucose tolerance” and “intolerance” really mean. It is not just about digestion, but how your body handles blood sugar right now and what this can mean long term.
We also discuss how to know if you are carbohydrate intolerant, ways it can show up, and how to figure out your tolerance. In the next article, we explore other factors that can affect how well your body handles carbs, how genes and lifestyle factors can play a role, and more.
What Is Carbohydrate (Glucose) Tolerance and Intolerance?
The terms carbohydrate tolerance or intolerance lack a scientific definition but are commonly used to describe someone’s reaction to consuming carbohydrates. Often, it is used interchangeably with glucose tolerance. Despite being closely linked, glucose and carbohydrate tolerance are not the same thing.
While this article focuses specifically on glucose tolerance and intolerance, it might be helpful to break down some of these other definitions:
Carbohydrate tolerance or intolerance refers explicitly to the body’s inability to properly process and metabolize foods that have carbohydrates, leading to negative health effects. More often than not, the term refers to food intolerances or negative reactions to the food rather than something to do with blood sugar. This can manifest in many ways. Here are some examples:
- Lactose intolerance is a form of carbohydrate intolerance that happens when your body doesn’t produce enough of an enzyme called lactose, which helps the body break down milk sugars.
- Fructose malabsorption impacts how well your body absorbs fructose; a carb commonly found in fruits, honey, and processed foods containing high-fructose corn syrup.
- Conditions such as Celiac disease, in which your immune system reacts poorly to proteins found in wheat products.
Also, under this umbrella, sometimes the term “carbohydrate intolerance” refers to glucose intolerance and insulin resistance, which are what we will be diving into below. But first, what does it mean to be glucose tolerant?
Glucose tolerance is your body’s capacity to regulate blood sugar levels after consuming glucose. When you consume a carb-containing meal, your body breaks them down into simpler, more absorbable glucose molecules, which can easily diffuse into the bloodstream.
When the body senses this, it releases a hormone called insulin to help transport glucose from the blood and into cells where it can be used for energy or stored for later.
Having good glucose tolerance refers to the body’s capacity to efficiently handle a certain amount of glucose without experiencing negative health effects.
People with good glucose tolerance can consume carbohydrates without significant spikes in blood sugar levels. Their bodies can produce enough insulin (a hormone that helps regulate blood sugar) and efficiently use the glucose for energy or storage.
On the other hand, glucose intolerance occurs when this normal process is impaired. It indicates that the body’s response to glucose is not as effective as it should be. People with glucose intolerance:
- Have a hard time regulating blood sugar levels
- May have elevated blood sugar for prolonged periods
- May need more insulin to bring down their blood sugar than a glucose-tolerant person, which can predispose them to post-meal blood sugar crashes. These crashes can manifest as irritability, fatigue, hunger, or cravings.
Glucose intolerance can also be a risk factor for metabolic syndrome and type 2 diabetes, when not managed effectively.
Finally, we have insulin resistance. Insulin resistance is closely related to glucose intolerance and occurs when your cells become less responsive to the effects of insulin. This can lead to poor blood sugar control. Glucose tolerance depends on sufficient insulin levels and sensitivity. If you don’t have enough insulin or insulin sensitivity, excess glucose remains in the bloodstream.
In summary, glucose tolerance refers to your body’s ability to regulate blood sugar levels after consuming glucose (which comes from the breakdown of carbs). Conversely, glucose intolerance is when your body struggles to maintain normal blood sugar levels after consuming glucose, which can impact your health.
Staying on top of your blood glucose values and maintaining normal glucose tolerance can be challenging, especially considering the daily fluctuations in glucose levels. Various factors, including diet, exercise, hormonal changes, sleep patterns, meal timing, medication, and stress, can all influence your blood sugar levels.
How to Know if I Am Glucose Tolerant?
Glucose tolerance exists on a spectrum, depending on multiple factors. A person with perfect glucose tolerance should have:
- Steady energy throughout the day, with no lulls or crashes, and not needing caffeine to get going
- Healthy and clear skin
- An easier time keeping hormones balanced
- A clear mind and overall happy mood
How Do I Know if I Am Carbohydrate (Glucose) Intolerant?

On its own, glucose intolerance does not usually cause any noticeable symptoms. Therefore, you should keep up with your routine checkups with your doctor (more on this below). However, some people might experience subtle symptoms that are related to unhealthy fluctuations in blood sugar levels, such as:
- Fatigue: Fluctuations in blood sugar levels can cause energy crashes, and lead to excess fatigue and weakness after consuming meals containing carbs. This is because high blood sugar disrupts how your body uses sugar for energy.
- Increased hunger: When the body cannot use glucose effectively for energy, it can cause increased hunger and food cravings.
- Excessive thirst: While common in diabetes, being more thirsty than normal can also indicate glucose intolerance. When too much sugar builds up in the blood, your kidneys must work harder to remove it in urine. When it does this, it also takes water out of your tissues, which can cause excess thirst and results in having to run to the washroom more often. This can also cause dry mouth.
- Blurry vision: High blood sugar can affect the fluid in your eyes, which can cause temporary changes in vision.
- Changes in weight: Poor blood sugar regulation can cause changes in weight, both increasing or decreasing it. Having poor insulin sensitivity can also cause more fat to accumulate in the stomach area.
- Mood changes: Fluctuations in blood sugar can impact mood and lead to irritability, stress, and even feelings of anxiety.
- Recurrent infections: high blood sugar can weaken the immune system. This can make you more susceptible to infections, especially urinary tract infections and yeast infections.
- Acne: High blood sugar, insulin, and IGF-1 can increase the likelihood of acne breakouts. While not everyone with acne has blood sugar issues, many clear up their skin once they adjust their diets to normalize their blood sugar.
These symptoms are not exclusive to glucose intolerance but can be warning signs that something else is going on. And some people with glucose intolerance experience no symptoms at all. Progressing symptoms can also indicate worsening glucose intolerance that is progressing toward prediabetes or diabetes, so it is important to undergo regular testing.
How Do I Find My Carbohydrate Tolerance?
If you are concerned about glucose intolerance, there are many methods that can help you determine whether you have it. Let’s look at what some of these tests are and how they are done:

Fasting Blood Glucose
This is a sample of blood that is taken after you fast for at least 8 hours. It is often used to screen for diabetes risk; however, it also has some downsides. It only provides a single point of measurement, which might not capture your full glucose metabolism.
It also does not assess how your body tolerates glucose following a meal. For example, this test won’t capture if you can have a fasting glucose that is within normal ranges, but experience high levels after you eat. It also does not consider any short-term factors that might impact levels, such as stress, sleep, and recent meals.
Importantly, low-carb or ketogenic diets can raise fasting blood glucose in healthy people, even though your blood sugar control and insulin sensitivity are improving. This is possibly because your organs and muscles start to rely on ketones and do not need as much glucose, leaving more in your blood.
Normal levels should be less than 100 mg/dL (5.6 nmol/L), while levels above that can indicate impaired glucose tolerance or prediabetes. However, some functional medicine doctors suggest that optimal values should be between 70-85 mg/dL, even though this can vary between different populations. For example, a study conducted in Korea found that ranges between 80-94 mg/dL were most beneficial for overall health.
Glycated Hemoglobin (HbA1C)
HbA1c is the portion of glycated hemoglobin or hemoglobin with glucose attached to it. This test estimates the average blood sugar levels over the past 2-3 months, which can provide more insight into glucose tolerance compared to fasting blood glucose.
This means it provides a more comprehensive view of glucose control. It is often used for diabetes screening and early detection. Compared to fasting blood glucose, HbA1C considers both fasting and post-meal blood sugar levels and is not influenced by short-term factors.
A normal level for this test is less than 5.7%, and any value between 5.7-6.4% can increase your risk for prediabetes or diabetes. Optimal values are 5.0-5.4%, with values lower than 4.0% linked to poorer health outcomes.
Glucose Tolerance Test
This test measures glucose levels before, and two hours after ingesting a sugary solution. The solution contains a specific amount of glucose (75 g) to see how well your body processes and regulates glucose. The test usually starts with a fasting blood sugar test, measured after an overnight fast to get your baseline measurement.
After consuming the glucose solution, your blood sugar levels are checked at regular intervals – 30 minutes, 1 hour, 2 hours, and sometimes 3 hours after. If your blood sugars are higher than normal, but not high enough to be in diabetic ranges, you might have impaired glucose tolerance.
This test can also be affected by things like stress, illness, medications, and even recent dietary changes. Because it only captures one day, it might not provide a complete picture, and abnormal levels often require another test to confirm them. Additionally, it only looks at how well your body responds to pure glucose, which might not reflect how you eat normally.
Homeostatic Model Assessment for Insulin Resistance
Homeostatic Model Assessment for Insulin Resistance (commonly referred to as HOMA-IR) is a calculation used to assess how sensitive your body is to insulin. In order to calculate this value, you need bloodwork that measures two things: fasting blood sugar, and fasting insulin. From there, HOMA-IR can be calculated quite easily.
If your HOMA-IR score is high, your body might not be able to use insulin efficiently, which could hint at insulin resistance. This can be a risk factor for developing type 2 diabetes or metabolic syndrome.
HOMA-IR scores can be elevated even before fasting blood glucose levels are high. In this situation, your body is working hard to maintain normal blood sugar levels. The pancreas is still producing insulin effectively, but pumping out higher volumes to ensure that glucose levels are controlled. This is one reason the HOMA-IR is a helpful tool for catching early cases of insulin resistance.
The higher your HOMA-IR score is, the more insulin resistant you are. Optimal values should be less than 1, with levels higher hinting towards signs of early insulin resistance.
Values greater than 2.9 suggest significant insulin resistance. However, there has been research on age variations in these values, and that is why it is always best to use HOMA-IR in combination with other tests in order to fully understand your unique risks.
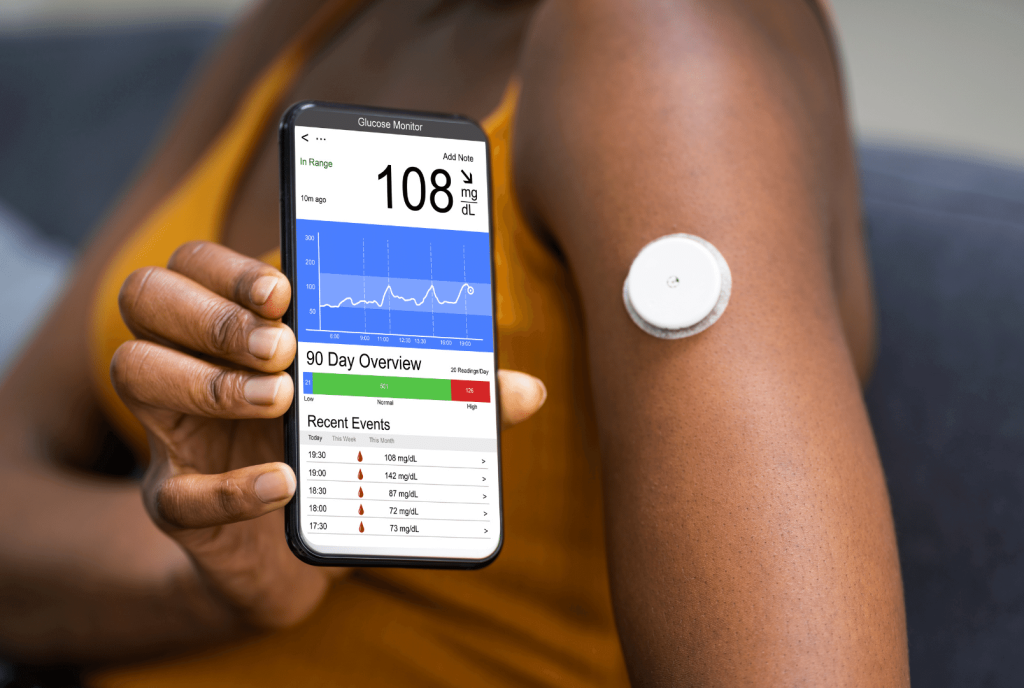
Continuous Glucose Monitoring (CGM)
CGMs are tiny sensors that are inserted under the skin, usually on the arm or belly. They measure the glucose fluid that is between cells, which can then be transmitted wirelessly to your phone or other device.
CGMs are helpful for monitoring glucose levels throughout the day and can help provide insight in real-time to help you understand the impact of lifestyle factors on your glucose control. With CGMs, it is like doing a glucose tolerance test multiple times per day while eating normally. You can track how your glucose levels respond to daily routines and provide you valuable information to adjust your lifestyle based on your results.
In this article, you’ve learned about glucose vs. carbohydrate intolerance, and ways to know if you may have it. In the next article, we’ll share about genetics, lifestyle contributors, and how to adjust your diet to improve your glucose tolerance.
References
- Manuals M. Overview of Lactose Intolerance.; 2023.
- Hantzidiamantis PJ, Lappin SL. Physiology, Glucose. StatPearls Publishing; 2022
- Goyal R, Nguyen M, Jialal I. Glucose Intolerance. StatPearls Publishing; 2023.
- Insulin resistance & prediabetes. National Institute of Diabetes and Digestive and Kidney Diseases. Published June 7, 2023. Accessed September 26, 2023. https://www.niddk.nih.gov/health-information/diabetes/overview/what-is-diabetes/prediabetes-insulin-resistance
- Kalra S, Sahay R. Diabetes fatigue syndrome. Diabetes Ther. 2018;9(4):1421-1429. doi:10.1007/s13300-018-0453-x
- Hardy K. Polyphagia – increased appetite. Diabetes. Published January 15, 2019. Accessed September 26, 2023. https://www.diabetes.co.uk/symptoms/polyphagia.html
- Diabetes and blurred vision. WebMD. Accessed September 26, 2023. https://www.webmd.com/diabetes/diabetes-blurred-vision
- Chiu CJ, Wray LA, Beverly EA. Relationship of glucose regulation to changes in weight: a systematic review and guide to future research. Diabetes Metab Res Rev. 2010;26(5):323-335. doi:10.1002/dmrr.1095
- Carey DG, Jenkins AB, Campbell LV, Freund J, Chisholm DJ. Abdominal fat and insulin resistance in normal and overweight women: Direct measurements reveal a strong relationship in subjects at both low and high risk of NIDDM. Diabetes. 1996;45(5):633-638. doi:10.2337/diab.45.5.633
- Penckofer S, Quinn L, Byrn M, Ferrans C, Miller M, Strange P. Does glycemic variability impact mood and quality of life? Diabetes Technol Ther. 2012;14(4):303-310. doi:10.1089/dia.2011.0191
- Atamna A, Ayada G, Akirov A, Shochat T, Bishara J, Elis A. High blood glucose variability is associated with bacteremia and mortality in patients hospitalized with acute infection. QJM. 2019;112(2):101-106. doi:10.1093/qjmed/hcy235
- Hasrat NH, Al-Yassen AQ. The relationship between acne vulgaris and insulin resistance. Cureus. 2023;15(1). doi:10.7759/cureus.34241
- Sadowska-Przytocka A, Gruszczńska M, Ostałowska A, et al. Insulin resistance in the course of acne – literature review. Postepy Dermatol Alergol. 2022;39(2):231-238. doi:10.5114/ada.2021.107101
- Yi SW, Park S, Lee YH, Park HJ, Balkau B, Yi JJ. Association between fasting glucose and all-cause mortality according to sex and age: a prospective cohort study. Sci Rep. 2017;7(1). doi:10.1038/s41598-017-08498-6
- Mukai N, Doi Y, Ninomiya T, et al. Cut-off values of fasting and post-load plasma glucose and HbA1c for predicting Type 2 diabetes in community-dwelling Japanese subjects: the Hisayama Study: Cut-off values of fasting and post-load glucose and HbA1c. Diabet Med. 2012;29(1):99-106. doi:10.1111/j.1464-5491.2011.03378.x
- Amanda. Why high fasting blood glucose on low carb or keto? –. Diet Doctor. Published October 13, 2017. Accessed September 26, 2023. https://www.dietdoctor.com/low-carb/fasting-blood-glucose-higher
- Carson AP, Fox CS, McGuire DK, et al. Low hemoglobin A1c and risk of all-cause mortality among US adults without diabetes. Circ Cardiovasc Qual Outcomes. 2010;3(6):661-667. doi:10.1161/circoutcomes.110.957936
- Glucose Tolerance Tests: What Exactly Do They Involve? Institute for Quality and Efficiency in Health Care (IQWiG); 2020.
- Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and ?-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28(7):412-419. doi:10.1007/bf00280883
- Freeman AM, Acevedo LA, Pennings N. Insulin Resistance. StatPearls Publishing; 2023.
- Abdesselam A, Zidoum H, Zadjali F, et al. Estimate of the HOMA-IR Cut-off value identifying subjects at risk of Insulin Resistance using a Machine Learning approach. Sultan Qaboos Univ Med J. 2021;21(4):604-612. doi:10.18295/squmj.4.2021.030
- Gayoso-Diz P, Otero-González A, Rodriguez-Alvarez MX, et al. Insulin resistance (HOMA-IR) cut-off values and the metabolic syndrome in a general adult population: effect of gender and age: EPIRCE cross-sectional study. BMC Endocr Disord. 2013;13(1). doi:10.1186/1472-6823-13-47
- Yamada C, Mitsuhashi T, Hiratsuka N, Inabe F, Araida N, Takahashi E. Optimal reference interval for homeostasis model assessment of insulin resistance in a Japanese population: HOMA-IR reference interval in Japanese. J Diabetes Investig. 2011;2(5):373-376. doi:10.1111/j.2040-1124.2011.00113.x
- Continuous glucose monitoring. National Institute of Diabetes and Digestive and Kidney Diseases. Published August 2, 2023. Accessed September 26, 2023. https://www.niddk.nih.gov/health-information/diabetes/overview/managing-diabetes/continuous-glucose-monitoring
